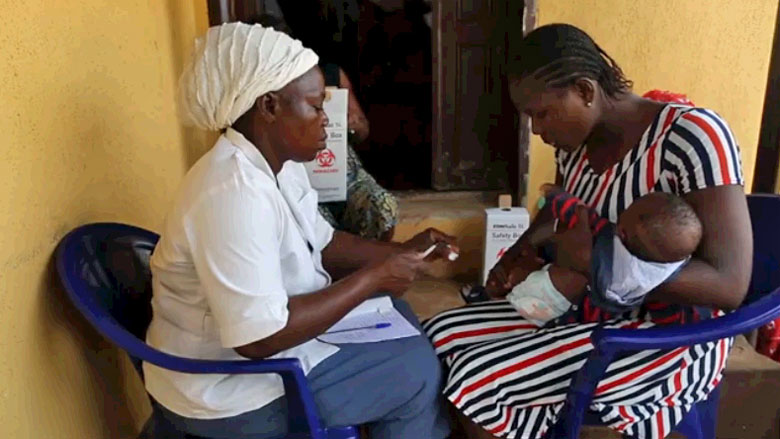
In Nigeria, more than one in 10 children will not survive to see a fifth birthday, and nearly one in 20 women will die in childbirth. In collaboration with the Government of Nigeria, researchers evaluated a program that aimed to save the lives of mothers and their babies by improving access to reliable health services and increasing the demand for these services.
| Research area: | Health Systems and Service Delivery |
| Country: | Nigeria |
| Evaluation Sample: | 250 Public Health Facility Clusters (four clinics per cluster) |
| Timeline: | 2013 – 2016 (Completed, endline report pending) |
| Intervention: | Incentives; Conditional cash transfer; training, supplies |
| Researchers: |
Pedro Rosa Dias, University of Sussex; Marcos Vera-Hernández, University College London; Marcus Holmlund, World Bank |
| SURE-P MCH research team: | Ugo Okoli, Project Director; Adetokunbo Oshin, Deputy Project Director; Sidi Ali Mohammed, Head of Health Workforce and Supplies; Chichi Aigbe, Operations Unit Lead; Jamila Bello-Malabu, Health Workforce Officer; Oluwafemi Adedipe, Head, ICT and Data Management; Chukwuebuka Ejeckam, Monitoring and Evaluation Officer; Chioma Oduenyi, Communications Officer; Nonso Onwudinjo, Communications Officer; Amina Muhtar, former Planning and Evaluation Lead; Laura Morris, former Planning and Evaluation Officer |
| Partners: | SURE-P Maternal and Child Health Program; National Primary Health Care Development Agency (NPHCDA); Nigerian Federal Ministry of Health; Development Impact Evaluation (DIME), World Bank; University of Sussex; University College London; Bill & Melinda Gates Foundation; Bank-Netherlands Partnership Program |
In many developing countries, pregnant women and infants are at risk of dying from often-preventable disease and complications related to pregnancy and birth. Prenatal care, midwife assistance and proper health facilities all help improve survival rates and ensure healthy births, but even such basic services are often not available or accessible to women in Nigeria.
Context
Nigeria, Africa’s most populous country, cut maternal and infant and child mortality by half between 1990 and 2008. Still, with an estimated 36,000 women dying annually in pregnancy or during childbirth Nigeria accounts for 13 percent of the world’s maternal deaths. Reasons include a shortage of trained midwives, low quality health clinics, high costs for patients, and low awareness of the importance of prenatal care and giving birth with a midwife or another trained health worker. The Government of Nigeria has been introducing reforms to improve health care. The evidence gathered from this impact evaluation can help policymakers in future maternal-child health care planning.