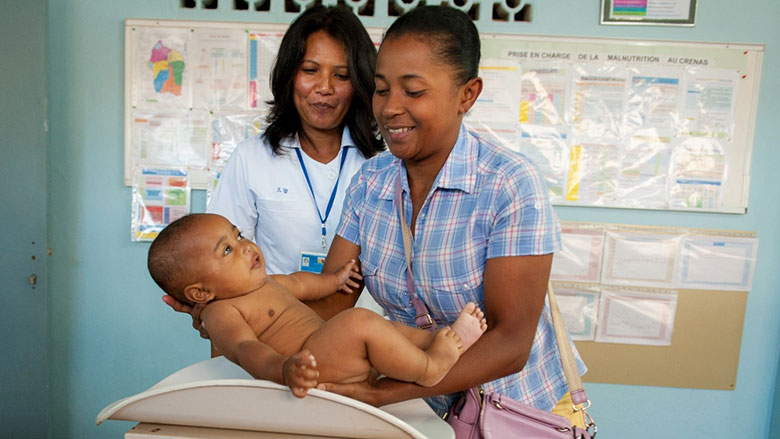
Challenge
In 2018, Madagascar had one of the highest rates of stunting in the world, with 42 percent of children affected; in some regions stunting rates were as high as 50-60 percent. Stunting – linked to poor healthcare, inadequate diets, and poor water and sanitation – is considered the biggest impediment to each child reaching her potential and the country’s socio-economic development. In 2016, the annual costs associated with malnutrition in Madagascar were estimated at 14 percent of the Gross Domestic Product (GDP).
Although global evidence has shown that a package of high-impact interventions can effectively reduce stunting, coverage of these essential health and nutrition services in Madagascar was limited and marked by substantial inequities. Despite the integral links between health and nutrition outcomes, primary care and community-based nutrition and health services were fragmented and uncoordinated. In 2017, only 35 percent of the target population was reached with nutrition services and distribution of qualified health care personnel was far below the World Health Organization’s (WHO)-recommended norms (less than three per 10,000 as of 2018 while the recommended standard is 23 per 10,000).
Moreover, the available services were of very poor quality; none of the clinicians interviewed during the Service Delivery Indicator (SDI) survey in 2016 correctly diagnosed five common tracer health conditions. Demand-side barriers included financial constraints, distance to facilities (55 percent of the population lived more than one-hour walk from a health facility in 2019), and lack of information about improved health and nutrition care and behaviors.
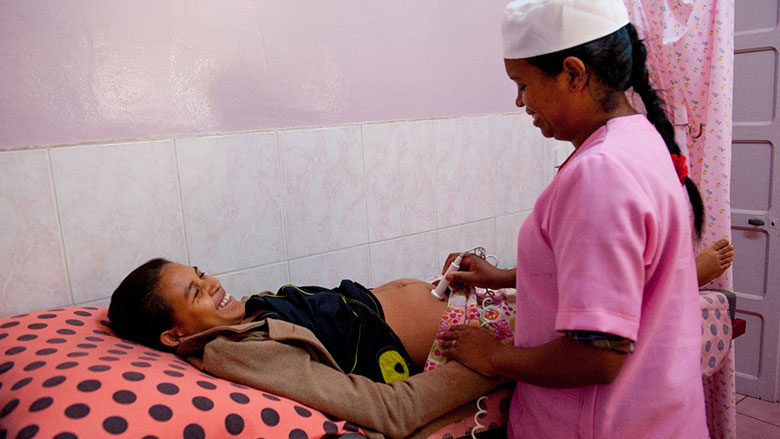
Approach
Significant improvements in a complex outcome like stunting require strengthening and transforming systems, beyond what can be achieved in the timeline of a single operation. The Madagascar Multiphase Programmatic Approach (MPA) is a 10-year $200 million International Development Association (IDA) program planned to be implemented in overlapping phases, with adaptive learning built in to maximize results. In this first phase, the project “Improving Nutrition Outcomes using the MPA” focused on rapidly accelerating results in the short term by increasing utilization of an integrated package of high impact Reproductive, Maternal and Child Health and Nutrition (RMCHN) interventions, and improving key nutrition behaviors known to be associated with significant reductions in stunting. The project focused on reducing fragmentation and increasing coordination of nutrition and health services while building systems to sustain outcomes in the longer term. The operation built on previous country experience and rigorous evaluations. The project team engaged global and local institutions with recognized expertise to ensure state-of-the-art technical assistance and forged new partnerships.
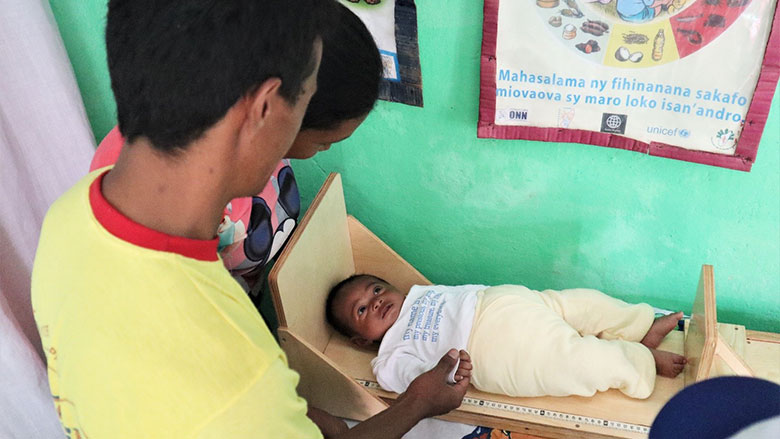
Results
The IDA financing supported a major effort of the government to bring the health and nutrition sectors together to deliver services in support of the multisectoral National Nutrition Action Plan III (2017-2021). This was the first time the health and nutrition sectors designed a joint program with a common goal. After two years of implementation (2018-2020), the first phase “Improving Nutrition Outcomes using the MPA” scaled up coverage and utilization of an integrated health and nutrition package at both community and health facility levels:
- More than 680,000 women and children received the newly approved RMCHN package of high impact health and nutrition services; 150,000 children fully vaccinated and nearly 500,000 women and children receiving nutrition services.
- Key indicators of health and nutrition services improved in project areas. Women attending antenatal care during their first trimester increased from 81,000 to 91,000; children treated for severe acute malnutrition increased from 870 to 5,600; and primary care facilities with tracer medications in stock increased from 296 to 700.
- 3,172 integrated health and nutrition community sites were established, and 465 primary health care facilities strengthened with necessary nutrition and health commodities and equipment to deliver the minimum RMCHN package.
- New approaches to improve competencies of service providers and quality of services. The health and nutrition sectors jointly developed the first standardized package of integrated nutrition and health services and an associated training curriculum. More than 6,000 community health workers and 977 health workers were trained using a new approach focused on practical sessions, continued supervision, and on-the-job training.
- To reduce barriers and increase utilization of health and nutrition services, the project scaled up the following innovations, building upon previous experiences in Madagascar and globally:
- A fee exemption scheme for key RMCHN interventions and project-financed delivery kits removed financial barriers to services.
- Distance barriers were reduced through vaccination outreach and delivery of Integrated Management of Childhood Illness and nutrition services through community sites.
- The significant constraint of available human resources for health was addressed by contracting health workers to increase alignment with Government norms, with an agreement that the new staff will be absorbed into the Government budget. The percentage of staff working alone in primary health-care facilities decreased from 46 percent to 32 percent (2018-2020).
- New partnerships and technical assistance were critical to bring in new thinking and best practices:
- The Government team visited Peru and Bangladesh to see firsthand how to achieve stunting reduction and strengthen nutrition services.
- Alive and Thrive developed a behavior-change communications strategy to improve prioritized nutrition behaviors based on cutting-edge research.
- The Medical Faculties and National Institute of Public Health in Madagascar developed an improved curriculum to improve quality of health professionals.
- Tanjaka Foods, a Malagasy private sector company, locally produced nutritional supplements that have historically been imported.

World Bank Group Contribution
The Madagascar MPA is a 10-year $200 million IDA program planned to be implemented in overlapping phases. The first phase (2018-2023) is a $80 million IDA grant.
Following the activation of the Contingency Emergency Response Component (CERC) in 2020 for rapid COVID-19 Emergency Response, $20 million in IDA was processed in additional financing to: ensure that originally planned activities under the project would be financed and implemented; mitigate the adverse impacts of the pandemic; and ensure the continuity of RMCHN essential services, especially routine immunization, safe deliveries and nutrition services.

Partners
- The first phase of the project was co-financed by The Power of Nutrition, with a $10 million grant.
- With the World Bank’s convening power and a longer-term commitment to the stunting reduction agenda through the MPA, synergies and partnerships were agreed with key development partners on other sectoral investments to maximize impact on stunting reduction:
- United States Agency for International Development (USAID) supported reproductive health and Water, Sanitation and Hygiene (WASH) with overlap in project areas. The project was co-located with USAID health support in one region, and there was an agreement on complementary financing to avoid duplication and ensure delivery of the minimum RMCHN package.
- The Japan International Cooperation Agency (JICA) supported nutrition-sensitive agriculture interventions with synergies with the community platform.
- The United Nations Children’s Fund (UNICEF) supported the decentralized management functions of the health system and complementary aspects of the nutrition agenda, including technical assistance and service delivery.
- The World Health Organization (WHO) provided technical assistance to improve the health information system. The Global Fund to Fight AIDS, Tuberculosis and Malaria and GAVI, the Vaccine Alliance, supported health system strengthening.
- Annual joint reviews with the Ministry of Health monitored progress towards achievements of sector development operational plans.

Moving Forward
- By 2023, the project will scale up to provide the minimum RMCHN package to nearly 2,090,000 children and over 650,000 pregnant women.
- Through the ten-year approach, the MPA will reach 75 percent of children in Madagascar with the minimum RMCHN package of services by 2028. Other partners are expected to align with the approach in support of the National Nutrition Action Plan. Successive phases of the MPA will progressively increase in geographical scale and in complementarity with other nutrition sensitive (multisectoral) interventions, such as social protection.
- Madagascar was selected as a Global Financing Facility (GFF) country in 2017 and will continue to make progress on its investment case and strengthening coordination on priorities in maternal, child and adolescent health and nutrition.
- The government of Madagascar further committed to the Human Capital agenda in March 2020 with the approval of $100 million in Investing in Human Capital Development Policy Financing. This is the first of two planned operations that introduces reforms to unblock key policy bottlenecks in human capital in Madagascar.
Beneficiaries
At a health center in a rural village in Itasy province, the program trained health workers on an integrated package of health and nutrition services and provided equipment and key commodities. A fee exemption scheme ensured that key maternal and child services were provided for free.
Dina, a mother of a newborn infant, explained: “They monitored my weight from the start of my pregnancy. And they advised me on healthy foods to eat. I came here regularly to have good health, to have normal weight for my baby, and to avoid complications during childbirth. My baby was very heavy, not like my other two babies. The first weighed 2.8 kilograms kg and the second one 2.6 kg. He weighed 3.5 kg.” Many residents in the catchment area have to walk more than an hour each way to reach the health center. The health worker, Lalasoa, added, “The service is free and it’s very important to people that it is free. So it increased the number of people coming.”