Challenge
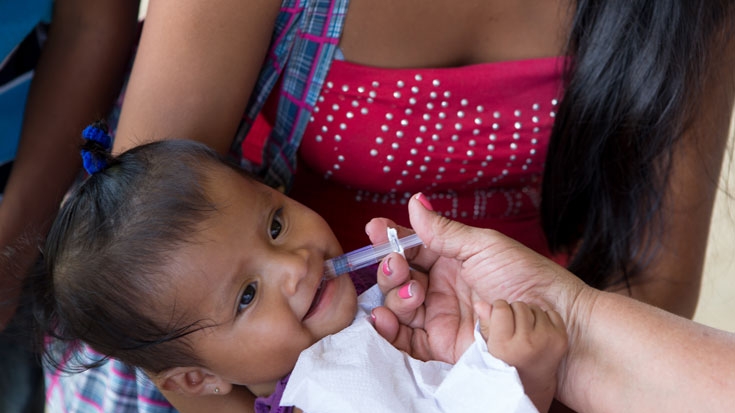
Panama’s key health sector challenge is to address inequitable health access for the poor while consolidating and scaling up existing incentives for the health system to improve the efficiency, effectiveness, and long-run sustainability. Individuals from rural poor and indigenous households experience lower health outcomes compared to other areas in Panama. Mortality rates for children under five years old in Bocas del Toro and the indigenous areas (comarcas) Ngobe Bugle and Kuna Yala are respectively 2.4, 1.9, and 1.6 times higher than the national average of 19.9 deaths per 1,000 live births.
In 2003, in an effort to address the issue of inequitable health access for the poor, Panama’s Ministry of Health (MOH) implemented an expanded national program to extend coverage of primary health care services (Estrategia de Extension de Cobertura – EEC) and increase access to health services. The expanded program included the delivery of the Integrated Package of Health Care Services (PAISS, for its Spanish acronym) to remote rural and indigenous areas using capitation payments that created financial incentives for providers to achieve better results, a results-based financing (RBF) approach. After five years of the PAISS experience, the MOH took the EEC to the next level by launching the Health Protection for Vulnerable Populations (PSPV) program which provided health services to the rural poor through mobile health teams. The PSPV was launched using an RBF approach supported through the Bank project which financed the capitation payments to the health regions which served as a financial incentive to increase coverage and improve performance.
Solution
The Bank embarked on an approach to help Panama address the inequitable health access for the poor through the design, launch, and implementation of the “Health Equity and Performance Improvement” (HEPI) Project in partnership with the MOH. Through the project a pair of complementary innovations were rolled out which included mobile health teams and the use of a results-based financing (RBF) approach. By financing mobile health teams, the project took away the burden of seeking health care from the rural poor and instead directly brought health care to the community. With regard to the RBF approach, the project financed capitation payments which consist of three tranche payments to networks of health facilities which enter into contracts with the MOH to provide services to the selected communities, through the mobile health teams. The first tranche is paid every two months (at the end of each health round) and can be a maximum of 65 percent of the per capita amount and is based on the achievement of target coverage levels. The second tranche, paid every 4 months, is for a maximum of 30 percent of the per capita amount and is paid according to achieving performance targets for health service provision among the registered beneficiary population. The third tranche is paid annually and accounts for 5 percent of the per capita amount based on a social audit which includes a survey among beneficiaries who received services to measure satisfaction levels.
At its start, the project suffered long delays in implementation due to factors outside the executing agency’s control. To provide a concrete solution to this problem, a first set of changes was made to the project in June 2012 which included: (i) extending the project closing date by 18 months to allow the project to have a full 5 years of provision of health and nutrition services through the mobile teams, (ii) introducing more flexibility in the percentage distribution of counterpart and loan funds for disbursements (the pari passu) across all project components, (iii) simplifying the disbursement conditions to allow capitation payments to be made against the certification of the beneficiary roster conducted by the external audit firm and not require a second certification which caused delays, and (iv) revising the targets of some indicators in light of baseline data. A second change was made to the project in October 2013 to respond to a significant reduction in funds assigned to the project for external and counterpart funds. This second change reallocated funds across categories to allow the project to maintain its current pace of implementation and finance the project’s central activity, the capitation payment for the provision of the basic package of health services to the target population of under-served rural communities.