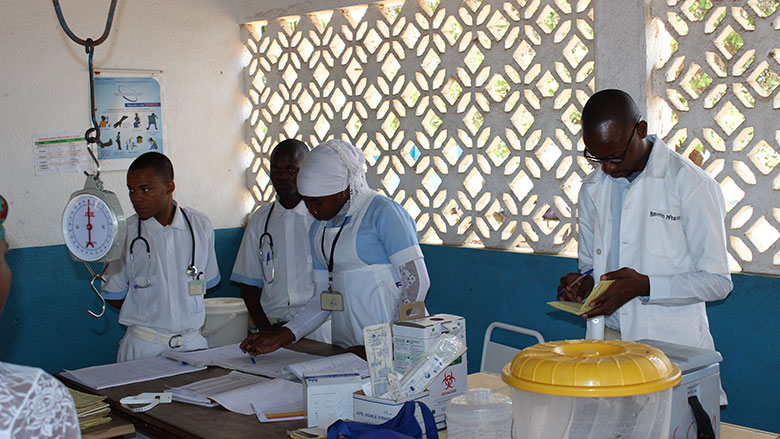
Prior to program implementation, inadequate planning for procurement, warehousing, and distribution practices led to recurrent medicine stockouts. Reports of stolen medicine sold in informal markets were recurrent. Expired or damaged medicines available in medical facilities were frequent, and above all, there was not enough medicine at service delivery points, resulting in poor quality of care and treatment outcomes.
“Medicines only have value when they reach the right patient at the right time,” said João Grachane, senior officer at the Ministry of Health, noting that the program helped improved the medicine supply chain.
This IDA-funded operation has shifted the attention from inputs to results among practitioners, decisively improving the medicine supply chain. Significant improvements in the health sector have been documented throughout implementation of the program; key progress includes a substantial increase in the availability of essential maternal health medicines at the facility level from 78.6% in 2013 to 86% to 2015, as well as a sharp decrease in the number of treatment sites with stockouts of antiretroviral drugs from 27% in 2013 to 5% in 2015.
In education, weak school governance, limited community participation, ineffective supervision, high absenteeism, and delays or diversions of school funds contributed to low pupil retention, low completion rates, and poor learning outcomes.
“We now receive our grants allocation at the beginning of the school year,” said Matilde Xilume, primary school director at EP1.2 of 3 de Fevereiro. “This is a major improvement as it allows us to plan better at the beginning of the year.”
Xilume said before the program, the grants were hardly allocated on time, which would disrupt the normal functioning of the schools. There are 1,300 primary schools under the program and all of them are benefiting from these improved allocations. The grant, known as ADE from its Portuguese acronym, is a budget allocated to schools to help improve learning conditions by providing basic learning materials. The grant also supports the most vulnerable children. Prior to 2014 the allocation of education grants to schools had never been accomplished on time. By 2016, 93% of complete primary schools had received their education grant by February, and most districts expenditures on education had been re-classified appropriately, to cite few examples.
The project, which is in its final stages of implementation, provided a unique support structure to create a network of reinforcing incentives. A timely capacity building window ensured that sectors collaborated with PFM agencies and had the resources they needed to deliver services and improve institutional capacity.
“The project adopted an innovative problem-driven and iterative approach towards implementation,” said Humberto Cossa, World Bank senior health specialist supporting the implementation of the health component. “Frontline implementers focused their attention on identifying bottlenecks to the achievement of results in their sectors, bringing people out of their silos to craft integrated solutions.” The project engaged a team of coaches and facilitators who were assigned to each of the participating ministries and in each province to support the coordination, behavior change and implementation discipline needed to reach the targets.
The program also helped the government improve the transparency and efficiency of spending on medicine distribution, storage, and availability as well as management of school councils, districts, and budget.
Looking ahead
Despite these and other advancements, Mozambique is still ranked 181 out of 188 countries in the Human Development Index, and it’s not yet on track to reach the health Sustainable Development Goals. It’s against this backdrop that in December 2017, Mozambique benefited from additional results-based financing totalling $105 million in non-reimbursable grants for the government of Mozambique’s Primary Health Care Strengthening Program‐for‐Results. Of this amount, $25 million equivalent is provided by the Global Finance Facility (GFF), and $80 million comes from the International Development Association (IDA). This new financing, which draws on the successful implementation of the 2014 Public Financial Management for Results Program, will focus on primary health care in underserved areas of Mozambique.