By Melanie Mayhew, Communications Officer, World Bank Group
In the windswept valleys of eastern Zambia, home deliveries are too common and some women die during childbirth.
But in Lundazi district, just steps from the border with Malawi, health facilities are using small incentives, like a drink, a few nappies, a colorful wrap, or a bar of soap, to encourage women to come to health facilities when they are pregnant, when they are about to deliver, when they need family planning services, and when they and their babies need checkups and vaccines.
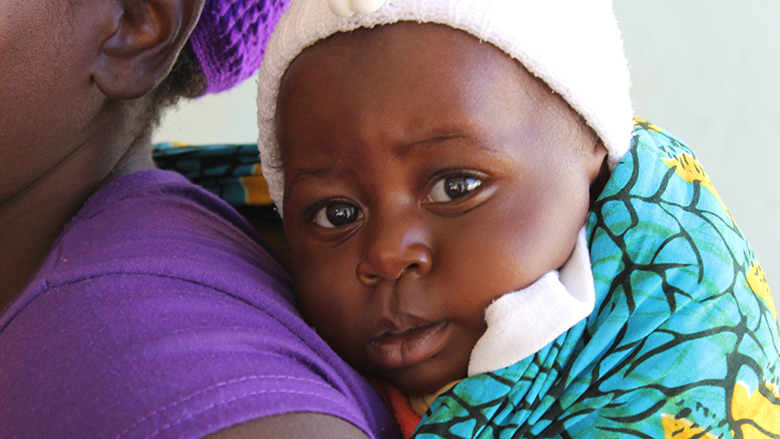
Mary, 21, rests on a bench outside of the Lundazi Urban Clinic, while her 6-month-old daughter, Rabbeca, sleeps in the wrap that encircles Mary. Mary, who is living with HIV, walked 7 kilometers to the clinic when she was pregnant with Rabbeca to have her baby tested for HIV. She took precautions to prevent her unborn baby from contracting HIV during pregnancy, childbirth and breastfeeding, and she is hopeful that this test, and another when Rabbeca is 1-year-old, will confirm that she is not infected with HIV.
When Mary became pregnant, she and her husband visited the health center, where they were each tested for HIV. When she received the results, she started taking antiretroviral medication to improve her health and prevent the virus from being transmitted to the baby. Then she returned for two more antenatal visits, delivered at the clinic, and has returned for her postnatal visits, which include family planning consultation. At each of these visits, Mary has received a small incentive, in addition to receiving the care she needs.
Mary had a safe pregnancy and delivery, and has a healthy child, because she came to the clinic throughout her pregnancy and to deliver her baby, after hearing that the health facility could offer her things that she could not get with a home delivery.
“I came here because the nurse has a very good attitude and the incentives they provide me, like the nappies,” Mary says.
These incentives are part of a results-based financing (RBF) approach that Zambia has implemented in more than 200 health facilities across the country. The aim is to address challenges like an insufficient and poorly motivated human-resource base, an erratic supply of essential medicines and medical supplies, limited autonomy in decision-making at health facilities, weak monitoring and evaluation systems, and poor quality of service delivery.
The Health Results Innovation Trust Fund at the World Bank supports the design and implementation of RBF approaches to accelerate progress in improving the lives of women, adolescents and children. In Zambia, RBF programs pay cash payments to districts and health facilities after pre-agreed results are achieved and independently verified.
RBF aims to increase autonomy, strengthen accountability, and empower frontline providers and health facility managers to make health service delivery decisions that best meet the needs of the women and children in the communities they serve. For example, money earned from the RBF is then used to pay staff motivation incentives, for investments at the health facilities, and for monetary and non-monetary incentives to consumers of health services.
One of these health care workers is Bridget Banda, a registered midwife at Lundazi Urban Clinic. She has worked at the clinic before and after the district introduced RBF.
“Now we have the knowledge and the skill and the motivation to attend to these women,” Banda says.
RBF has led to a culture change that is benefitting health workers and the communities.
“I always refer to it as the RBF culture of excellence where staff were motivated to always look forward to excellence. They wanted to be on top … [and] they were motivated through bonus incentives,” says Allan Chisenga, the district medical officer for Lundazi district.
Implementing RBF has also helped train staff in business planning and data collection—and has encouraged staff to take action after reviewing these results, Chisenga says.
“RBF” is spray-painted on many of the things that the clinic has purchased with RBF funds: the water pump, chairs, the generator that ensures that vaccines are kept cold, the TV that attracts patients to the clinic, the shelter where women like Mary wait to be examined after walking from afar. The health workers provide maternal and child health care in the shelter, as well as perform male circumcisions there every Friday. RBF also funded the tuck shop, where patients buy groceries, the profits of which help offset the clinic’s operational costs.
The clinic’s motorbike and bicycles also include the “RBF” imprint. Health workers use the bikes to bring pregnant women to the facility, and to travel to far-flung communities to immunize children. All of these things, as well as the bonuses, cleaning supplies, electricity, drugs and patient incentives that RBF has financed are changing how the community views and invests in health.
Before RBF, in-facility (institutional) deliveries were low at Lundazi Urban Clinic—women delivered at home. Now, there are about 80 deliveries at the clinic each month. Early results from an impact evaluation of the country-wide RBF program indicate that RBF has significantly increased use of some maternal and child health services. Women from health facilities in RBF districts sought antenatal care about two weeks earlier than women in non-RBF districts. The rate of in-facility deliveries also increased by almost 13%.
“This has really led to a reduction of maternal deaths in the community because most of the people are coming for institutional deliveries now,” Banda says.
In Chinombo Village in Lundazi, villagers perform a skit in which a woman asks her husband to go to the health facility to get tested for HIV, and the man encourages his wife to go to a health facility to deliver their baby. This community-driven education is one of the ways that facilities contracted by the RBF program raise community awareness about their services.
“I tell my people that the best place to seek medical help is at the health facility,” says David Mwanza, a village chief.
Before RBF, in one year, seven women died when they tried to deliver their babies at home.
Community members like Beatrice Thole, who participates in the community’s Safe Motherhood Action Group (SMAG), have taken responsibility for ensuring that women go to their antenatal and postnatal visits and deliver in a health facility. Thole used to be a traditional birth attendant who helped women deliver at home.
“After learning the importance of delivering at the health facility, I started encouraging and accompanying women to the health facility,” Thole says.
She receives no salary for her work—but for every five women she takes to the health facility, she receives a small payment, and respect from Chinombo villagers.
These efforts by entire communities are paying off: In addition to more women delivering in facilities, postnatal care coverage and immediate breastfeeding have increased.
Building on the positive experiences of RBF and the Health Results Innovation Trust Fund across many countries, the World Bank Group and partners has now launched the Global Financing Facility in support of Every Woman Every Child, a country-driven financing partnership that will provide smart, scaled and sustainable financing to accelerate efforts to end preventable maternal, newborn, child and adolescent deaths by 2030.