By Kate Mandeville, Vikram Rajan, Aparnaa Somanathan, Anthony Oundjian, Emily Serazin, and Qahir Dhanani
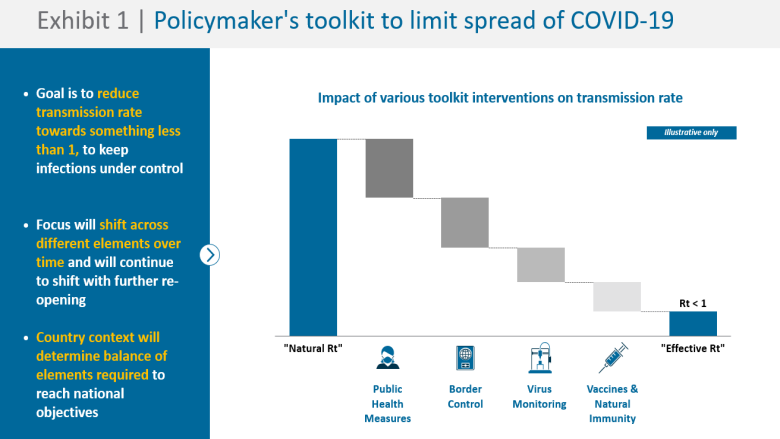
When COVID-19 hit East Asia and the Pacific (EAP) in early 2020, many countries in the region successfully limited its spread through aggressive deployment of tools such as public health measures, border controls, and monitoring systems. (Exhibit 1.) As the pandemic continues, however, the continued application of these tools is challenging, as can be seen from recent surges in Vietnam, Thailand, and Singapore. Supply constraints mean that many countries may not fully vaccinate their populations until 2024, even as new variants emerge against which existing vaccines may be less effective. Beyond the targeted response, many countries are now looking to defray the accumulated costs of the pandemic through re-opening and rejuvenating their economies and societies.
With such a dynamic situation, countries need to continuously learn from each other and adapt their responses as new tools become available. The recently concluded COVID-19 Workshop Series was an opportunity to hear from global and regional experts about different approaches to “respond, re-open, and rejuvenate” in EAP. Over the course of the series, seven key themes emerged:
(1) We are in a race between vaccines and variants
More transmissible new variants may overwhelm health systems and/or render vaccines less effective, creating the imperative for a globally coordinated response.
(2) The policymakers’ toolkit has expanded, and choosing between these tools has become more complex
Vaccination, while critical, is an addition to the original COVID-19 response toolkit. The emergence of new tools may lead to the evolution of others, such as the addition of vaccine passports to border measures. However, the virus’ ability to fight back means that more sophisticated versions of the original tools are also needed, such as genomic surveillance to track variants.
(3) The endgame remains clear, with endemic or zero COVID-19 both possible scenarios for the region
Some experts argue that the convergence of (1) vaccines not providing sterilizing immunity; (2) new variants’ increasing transmissibility; and (3) vaccine hesitancy limiting high vaccine coverage may result in an endemic COVID-19 scenario. Others point to the success of EAP countries in achieving elimination through crush and contain strategies and argue that elimination may be possible in the longer term through high levels of vaccination.
(4) Proponents of both scenarios agree on the critical importance of rapid vaccination
At the global level, further redistribution of resources via COVAX (including funding for procurement and vaccine donations) is critical to ensure supply availability. In parallel, countries can prepare for high throughput before supplies arrive, especially given the sharp increase in COVAX supply volumes that is anticipated in the second half of 2021. On the demand side, policy makers must demonstrate trustworthiness, clearly communicate the risks and benefits for individuals, and emphasize community as well as individual benefits.
(5) Vaccination rollout and other tools to combat COVID-19 can provide entry points for addressing neglected health system challenges.
The lessons learned from the pandemic point to the critical importance of strengthening of public health systems and fast-tracking universal health coverage. This agenda can leverage the data and delivery systems demanded by vaccination rollouts.
(6) Countries will need to make difficult choices and trade-offs against a backdrop of constrained fiscal space
We know that the economic impact of COVID-19 has not only hurt government revenues and budgets, but also household employment and income levels. Countries can efficiently utilize scarce resources by leveraging global and regional infrastructure (e.g. regional surveillance networks in Africa and the Caribbean), partnering with local universities and the private sector, transitioning from campaign mode to routine services, and leveraging COVID-19 financing for broader investments in health systems strengthening.
(7) Adaptive policymaking will be a critical success factor
Developments surrounding variants, vaccine effectiveness, and vaccination strategies are being reported daily. For example, several countries have now approved COVID-19 vaccination for adolescents. Others are considering booster shots and matching and mixing vaccine formulations. This rapid evolution means that adaptive policymaking – an approach which is flexible, data-driven, and responsive to emerging best practice will be critical to exiting the acute phase of the pandemic.
Overall, there are reasons for optimism, with vaccination accelerating as supply constraints ease and a unique opportunity to build stronger and more resilient health systems. Countries will need to continuously adapt their toolkit in a context of constrained fiscal space and growing complexity. As the pandemic has repeatedly shown us, this will require collaboration and solidarity at regional and global levels. No one is safe until everyone is safe.
Click here to download a full version of the summary
Last updated: July 2021