Chikungunya fever is spreading more rapidly through Latin America and the Caribbean than it takes to learn to spell and pronounce its name correctly.
The virus has already killed 21 people and infected some 6,000 in the region, a relatively small number compared with similar diseases. However, experts are concerned that Latin Americans still have not developed antibodies against the disease given its recent appearance.
In other words: the entire Latin American population is at risk of infection.
Like Ebola, which is now a global problem, chikungunya originated in Africa. In the local Makonde language, the name of the disease means “to double over in pain.” On that continent, the first outbreaks were reported in 2004. The virus has since spread to Oceania, Southeast Asia and parts of Europe.
And now it has arrived in Latin America.
The first cases were detected in late 2013. So far, an estimated 500,000 people have contracted it, mainly in the Caribbean. The virus spreads quickly: it has now reached southern South America with two confirmed cases in Argentina.
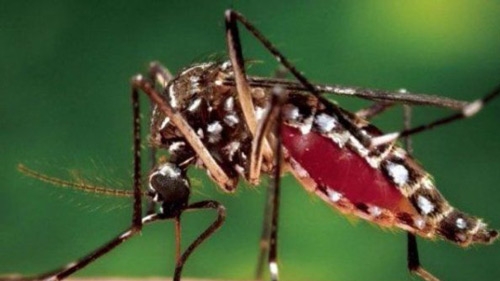
That is not surprising given that the vector of the chikungunya virus is Aedes aegypti, the same as dengue fever, a familiar nemesis in the region. Dengue affected more than 2.3 million people last year alone.
Fernando Lavadenz, a World Bank health expert, explains why cases have increased in Latin America and the Caribbean and what measures governments can adopt to control it.
Question: Why does this disease seem to “travel” more quickly than other viral diseases?
Answer: We are in a century of migrations and frequent travel, and consequently, in a context where disease spreads rapidly. To date, 30 countries in the Americas have been affected – Argentina is the most recent – and the majority of cases are “imported.”
To give you an idea, every year, nine million people travel to the Caribbean Islands, where chikungunya first appeared in the region, from the United States alone. Undoubtedly, some of these people do not take precautions and are bitten by the Aedes aegypti mosquito. When they return to their country in the viremic stage – with the virus in their bloodstream – they become potential transmitters of the disease when bitten by mosquitos that do not have the virus. This propagates the disease. Today there are native cases resulting from that process.
Additionally, this disease did not previously exist in the region, for which reason 100 percent of the Latin American and Caribbean population is susceptible to it. In other worlds, there is no record of antibodies to chikungunya and no natural resistance to the disease. Consequently, infection via mosquito is extremely high. Finally, the fact that Aedes aegypti is the same vector as dengue means that countries with high rates of that disease also will be vulnerable to chikungunya.